Debunking the Myth of Effortless Success in Aesthetic Medicine
In this article, Dr Rhead – an NHS doctor who has transitioned into medical aesthetics – examines the…

Understanding Pigmentation, Inflammaging and Midlife Skin Changes.
Consultant pharmacist prescriber Mary Keltai explores the science behind pigmentation, the role of inflammaging, and how
skin changes during midlife.
When patients over 40 attend clinics asking for advice about their skin,
this is where a robust consultation carries so much weight. There are
several aspects that can impact the ageing process – noticeably affecting the skin – as the most visible organ in the body. At this stage of life all patients around this age, regardless of ethnicity, may notice these little changes that can cause so much concern.
Inflammaging vs Inflammation
Inflammaging is a major driver in the process of ageing affecting the appearance of pigmentation, wrinkles and skin quality (1).
This raises an important question: what is the difference between inflammation and inflammaging?
Inflammation is our friend and is a natural response that the body has to trauma, infection and toxins leading to recovery. This is achieved
through the release of a complexity of both pro-inflammatory and anti-inflammatory cytokines and growth factors which help the
healing and regeneration of tissue.
Inflammaging on the other hand is a process of low-grade chronic inflammation which is persistent and driven by co-morbidities,
medication, mitochondrial dysfunction, immune dysregulation, senescence and oxidative stress (2,3).
Change in hormones, for example, in women over 40 – beginning at perimenopause – is where inflammation slowly increases (4). The
impact of inflammaging is cellular fatigue compromising the function of lipids proteins and DNA, and can exacerbate flare ups of
autoimmune diseases.
Immune dysregulation can have significant consequences, particularly as patients age. For example, individuals may begin to experience flare-ups of conditions like psoriasis due to their genetic
predisposition5. This is often seen when family members have a history of a skin disease and as the immune system weakens with age, it can trigger a flare-up even in individuals who have never had such skin
concerns before (3).
Ageing skin is not simply about drier and thinner skin. It is about collagen breakdown, compromised barrier function, increased
melanocyte reactivity and more potential for PIH (Post Inflammatory Hyperpigmentation) (6,7).
Pigmentation
Melanin released by specialized skin cells called melanocytes, is a natural photoprotective mechanism to protect the DNA within the
nucleus of our skin cells when exposed to triggers such as UVR, pollution, hormones and inflammation (8,9). Cutaneous inflammation may be precipitated by multiple factors, including procedural trauma from medical devices and, in some cases, pharmacological agents.
DNA damage entails distortion of the DNA helix leading to cell mutations, chronic skin aging, lesions and skin cancers like melanomas
and carcinomas such as BCCs and SCCs10,11.
There are two types of melanin released by the melanocytes: eumelanin a brown to black pigment which is very photoprotective and the
lighter phaeomelanin red to yellow pigment which is less UV protective and more prone to oxidative stress generation8. The ratio of
phaeomelanin to eumelanin contributes to phenotype but it is not the whole story.
In 1975 dermatologist Thomas Fitzpatrick created the Fitzpatrick Skin Phototype Scale Types 1-VI based on the patient’s tendency to burn, ability to tan and baseline pigmentation (12).
It has been established that genetics play a predetermined role in how darker skins respond to trauma and why darker patients are more prone to melasma (13). In Fitzpatrick IV–VI the inflammatory
mediators (prostaglandins, cytokines and leukotrienes) cause a stronger
melanocyte reactivity (7). This has the effect of accelerating an already more active melanin production and in this case the melanin pigment is the darker eumelanin since eumelanin is the dominant pigment pathway for these patients.
As we age neighbouring melanocytes do not respond equally leading to a generally mottled and uneven pigmentation. This is explained
by the fact that melanocyte activity declines as we age by 20-30% every decade after the age of 30 but the remaining melanocytes may
enlarge displaying heterogenic effects (6).
Traditional treatment options
Before modern dermatology, pigmentation disorders were treated with plant-based and mineral preparations such as Lemon juice, Sour milk (containing lactic acid), Citrus extracts (natural acids) and these worked
mildly through gentle exfoliation, surface lightening and anti-inflammatory effects.
Since the 1960s, the introduction of tyrosinase inhibitors such as Hydroquinone has marked a new era in treatment. These agents are considered the gold standard, often used alongside retinoids, exfoliants, and chemical peels for optimal results.(14,15).
Several treatment options are now available, but early prevention – especially through the use of sunscreen and antioxidants to reduce inflammation – is fundamental. The key to long-term success is about prevention, correction and maintenance and reducing triggers for melanocyte activation.
Tyrosinase inhibitors have been used for centuries in Asian populations natural tyrosinase-inhibiting botanicals such as Arbutin (from bearberry/mulberry) Kojic acid (from fermented rice/mushrooms) Glabridin (from liquorice) Ellagic acid (from berries) (16).
The tyrosinase enzyme itself wasn’t understood until modern biochemistry where these botanicals were identified as tyrosinase inhibitors reducing melanin synthesis and acting as antioxidants (16).
Case Study:
Patient assessment – Pigmentation
A 45-year-old female patient, Fitzpatrick II, presented with a concern of pigmentation and skin quality. Listening to the patient’s account of her distress regarding the worsening pigmentation during the summer
months created an opportunity to explore the underlying reasons for this seasonal exacerbation.
UVB rays (280–320 nm) are more prevalent in the summer months in northern latitudes due to clear skies and good weather and
less absorption due to reduced atmospheric scattering. UVA (320–400 nm) on the other hand are constant all year round as they penetrate clouds and glass, and this is the reason why we need to protect our skin with sun protection and antioxidants all year round(11).
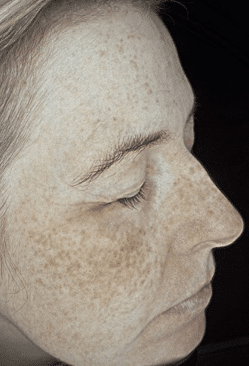
Before

After
UVA leads to instant skin darkening without creating new melanin. It induces immediate pigment darkening through oxidation of pre-existing melanin and generates reactive oxygen species that contribute to photoaging. However, UVB stimulates the synthesis of new melanin, and this is where a tyrosinase inhibitor regulates how a melanocyte responds to trigger mechanisms regulating the release of melanin (9,11).
It is important to explain to the patient how the following products contribute to the overall treatment plan, and to emphasise the
role of ongoing maintenance in achieving sustained, long-term results.
Clinicians work with many key algorithms that include:
During the consultation process it is important to use skin scanners to assess inflammation, the degree of underlying pigment distribution and barrier health, adjusting protocols to minimise risk before
initiating active treatments.
Pigmentation in midlife is multifactorial driven by inflammaging, UV exposure and melanocyte dysregulation. With thoughtful consultation and realistic goal setting, we can achieve meaningful improvement while protecting long-term skin health (18).
Understanding the triggers of pigmentation is fundamental to developing bespoke treatment pathways tailored to each patient. It is essential to emphasise the importance of year-round photoprotection and to frame treatment not solely as short-term correction, but as part of a long-term strategy for pigment control and maintenance.
References
1.Pilkington SM, Bulfone-Paus S, Griffiths CEM, Watson REB. Inflammaging and the skin. Exp Dermatol. 2021;30(7):1003-1014.
2.Franceschi C, Garagnani P, Parini P, Giuliani C, Santoro A. Inflammaging and ‘Garb-aging’. Trends Endocrinol Metab. 2018;29(9):623-633.
3.Fulop T, Witkowski JM, Olivieri F, Larbi A. Immunosenescence and inflamm-aging. Clin Interv Aging. 2018;13:239-250.
4.Verdier-Sevrain S. Effect of menopause on the skin. Climacteric. 2017;20(1):1-7.
5.Griffiths CEM, Armstrong AW, Gudjonsson JE, Barker JNWN. Psoriasis. Lancet. 2021;397(10281):1301-1315.
6.Tobin DJ. Introduction to skin aging. J Tissue Viability. 2017;26(1):37-46.
7.Davis EC, Callender VD. Postinflammatory hyperpigmentation: a review. J Clin Aesthet Dermatol. 2017;10(7):14-23.
8.Slominski AT, Zmijewski MA, Plonka PM, Szaflarski JP, Paus R. Melanin pigmentation in mammalian skin and its hormonal regulation. Physiol Rev. 2018;98(3):1153-1228.
9.D’Orazio J, Jarrett S, Amaro-Ortiz A, Scott T. UV radiation and the skin. Int J Mol Sci. 2019;20(19):4842.
10.Cadet J, Douki T. Formation of UV-induced DNA damage contributing to skin cancer. Photochem Photobiol Sci. 2018;17(12):1816-1841.
11.Narayanan DL, Saladi RN, Fox JL. Ultraviolet radiation and skin cancer. Int J Dermatol. 2016;55(1):1-7.
12.Gupta V, Sharma VK, Kaur I. Fitzpatrick skin phototype classification revisited. Clin Dermatol Rev. 2019;3(2):65-72.
13.Passeron T, Picardo M. Melasma and hyperpigmentation disorders. J Am Acad Dermatol. 2018;78(3):581-593.
14.Mukherjee S, Date A, Patravale V, Korting HC, Roeder A, Weindl G. Retinoids in the treatment of skin aging. Clin Interv Aging. 2016;11:175-182.
15.Bandyopadhyay D. Topical treatment of melasma. Indian J Dermatol. 2021;66(4):373-381.
16.Smit N, Vicanova J, Pavel S. Tyrosinase inhibitors in cosmetic dermatology. J Dermatol Sci. 2020;98(2):75-81.
17.Passeron T. Tranexamic acid in melasma. Dermatol Surg. 2020;46(8):1123-1126.
18.Passeron T, Picardo M. Melasma and hyperpigmentation disorders. J Am Acad Dermatol. 2018;78(3):581-593.
Gain full access to peer-reviewed protocols, our extensive digital archive, and the Tri-annual print edition delivered to your clinic.
£
250
Per Year
Subscribe
Auto-renews annually. Cancel anytime.
Subscribe to our newsletter for the latest insights from the aesthetics industry.
Subscribe Now