Roseway Labs and Mast Cell Action Unite to Advance MCAS Education
Leading UK compounding pharmacy Roseway Labs has officially announced a strategic partnership with Mast Cell Action, a UK-based…

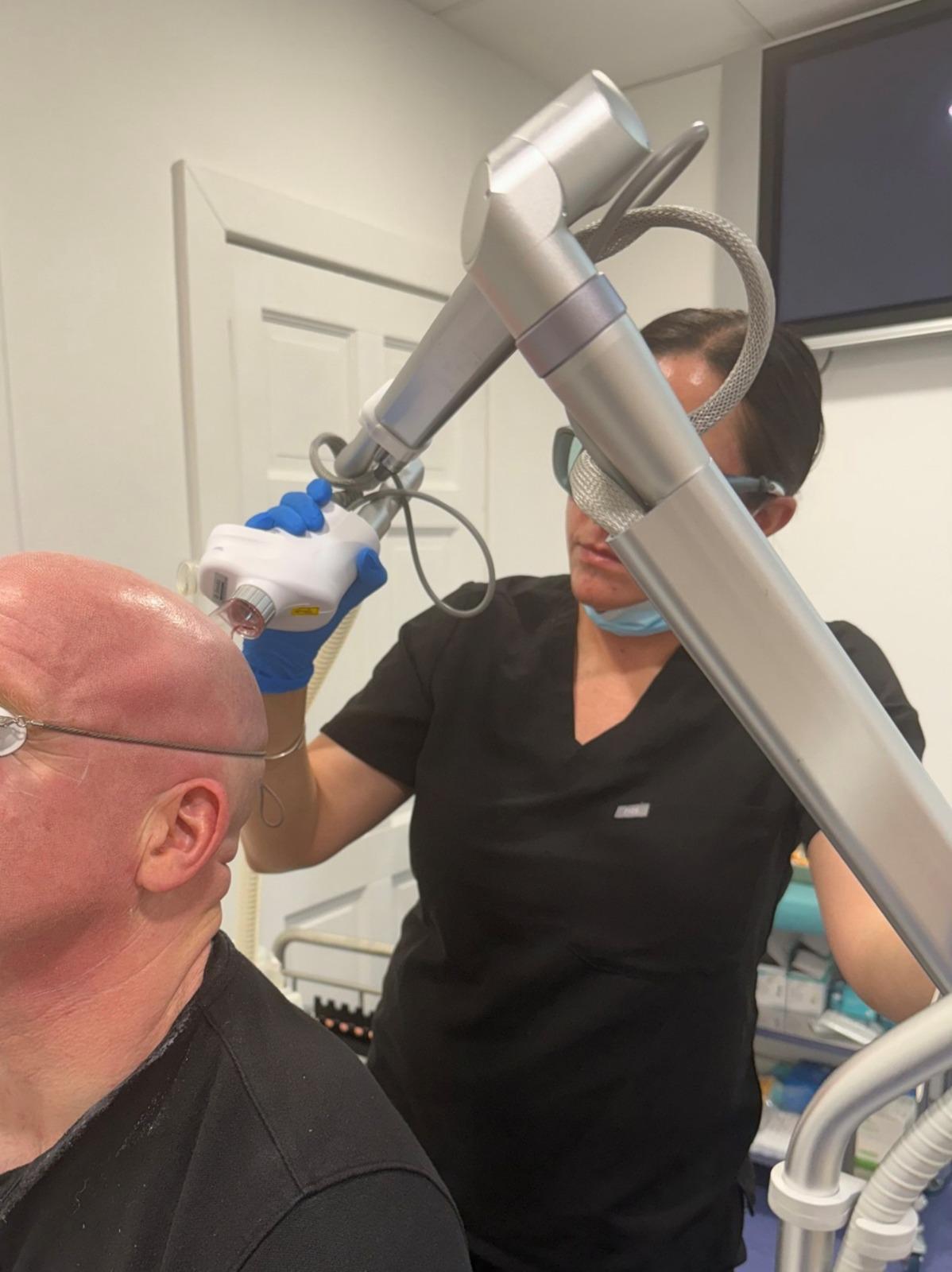
Professor Patrick Treacy explains how fractional CO2 laser pre-treatment and dual-wavelength illumination are enhancing lesion clearance, improving field treatment, and refining outcomes in sun-damaged skin.
Actinic keratosis (AK) is one of the most common precancerous skin conditions seen in dermatology. It arises from years of cumulative ultraviolet exposure and is particularly prevalent on sun-exposed areas such as the face and scalp.
While individual lesions may appear small and innocuous, their biological significance is important: untreated lesions carry a measurable risk of progression to squamous cell carcinoma.
For this reason, dermatologists increasingly favour field-directed therapies – treatments designed to address not only visible lesions but also the wider area of sun-damaged skin in which abnormal cells may already be developing.
Among the most established of these treatments is photodynamic therapy (PDT).
The Science Behind Photodynamic Therapy
Photodynamic therapy works through a deceptively simple biological principle. A photosensitising compound – commonly 5-aminolevulinic acid (ALA) or its methylated derivative methyl aminolevulinate (MAL) – is applied to the skin. Dysplastic keratinocytes preferentially absorb the compound and convert it into protoporphyrin IX (PpIX), a light-sensitive molecule.
When exposed to specific wavelengths of light, PpIX produces reactive oxygen species, which selectively destroy abnormal cells while sparing surrounding healthy tissue. PDT has been widely used for actinic keratosis for many years, offering several advantages over destructive techniques such as cryotherapy.
In addition to treating the entire field of sun-damaged skin, PDT typically produces excellent cosmetic outcomes with minimal scarring or pigmentary change. Yet, despite its effectiveness, traditional PDT protocols have limitations. One of the key challenges lies in photosensitiser penetration, particularly in thicker or more advanced lesions.
Enhancing PDT with Fractional Laser Technology
Recent advances in dermatological technology have focused on improving the delivery of photosensitisers into the epidermis. One promising strategy is fractional CO2 laser pre-treatment, which creates microscopic channels in the skin that allow topical compounds to penetrate more effectively.
By selectively ablating portions of the stratum corneum, fractional lasers facilitate deeper absorption of ALA or MAL and promote greater accumulation of protoporphyrin IX in abnormal keratinocytes.
Clinical experience suggests that this laser-assisted approach can significantly enhance the efficacy of PDT, particularly in patients with moderate to severe actinic keratosis.
Dual-Wavelength Illumination
Another area of innovation involves the wavelength of light used to activate the photosensitiser. Protoporphyrin IX has several absorption peaks, most notably in the blue spectrum (around 415 nm) and the red spectrum (around 630–635 nm). Blue light is highly effective at activating PpIX in superficial epidermal layers, while red light penetrates deeper into tissue.
Combining both wavelengths may therefore offer a theoretical advantage—treating lesions at multiple depths simultaneously. In a recent clinical series involving patients with moderate to severe actinic keratosis of the face and scalp, fractional CO2 laser pre-treatment was combined with topical photosensitisers followed by LED-based photodynamic therapy.
Patients received either dual-wavelength illumination (red followed by blue light) or blue-light-only PDT, allowing comparison between the two approaches. The outcomes were striking. At three months following treatment, lesion clearance rates reached 96% in the dual- wavelength group and 94% in the blue-light-
only group, demonstrating excellent clinical effectiveness for both protocols.
Patient satisfaction was similarly high, with most participants rating the cosmetic and clinical outcomes as very satisfactory.
Although transient erythema was common—an expected inflammatory response to PDT – it typically resolved within one week. No severe adverse events were observed. Pain during illumination was somewhat
greater in the dual-wavelength protocol, likely reflecting deeper activation of the photosensitiser and increased production of reactive oxygen species. The high clearance rates observed with this approach appear to reflect two complementary mechanisms.
First, fractional laser pre-treatment increases photosensitiser penetration, allowing greater accumulation of protoporphyrin IX within dysplastic cells. Second, dual-wavelength illumination activates PpIX across multiple tissue depths, improving the treatment of thicker lesions that might otherwise respond less well to conventional PDT. Together, these innovations suggest that laser-assisted PDT may represent a particularly valuable strategy for patients with more advanced or resistant actinic keratosis.
The Dermalux Tri-Wave MD is a frequently used LED device for photodynamic therapy in the treatment of actinic keratosis.
Advantages Over Conventional Therapies
Compared with traditional field treatments such as 5-fluorouracil or imiquimod, photodynamic therapy offers several practical
advantages:
Gain full access to peer-reviewed protocols, our extensive digital archive, and the Tri-annual print edition delivered to your clinic.
£
250
Per Year
Subscribe
Auto-renews annually. Cancel anytime.
Subscribe to our newsletter for the latest insights from the aesthetics industry.
Subscribe Now